The Critical Role of Routine Dental Exams
Routine dental exams are a defense against oral cancer. During each visit the dentist performs a tactile inspection, looking for white or red patches, non‑healing sores, and lumps that may signal early disease. By discussing tobacco, alcohol, HPV and sun exposure, clinicians empower patients to understand their risk and adopt new habits. Check‑ups catch lesions when they are small, increasing the chance of curative treatment and preserving quality of life.
Why Regular Exams Matter for Early Detection
Why Regular Exams Matter for Early Detection
| Benefit | Details |
|---|---|
| Early detection | Visual‑tactile exam of lips, tongue, gums, cheeks, floor/roof of mouth, and neck. |
| Risk‑factor assessment | Tobacco, alcohol, HPV, age > 40, family history → determines screening frequency (annual or 6‑month for high‑risk). |
| Survival advantage | Detecting localized disease → 5‑year survival 80‑90 % vs 30‑40 % for advanced disease. |
| Guideline | ADA recommends ≥1 oral‑cancer screen per year for all adults; more frequent for high‑risk. |
| Self‑exam synergy | Monthly self‑exams catch changes between visits, prompting timely biopsy. |
 Routine dental visits are the frontline defense against oral cancer. Every comprehensive check‑up includes a visual‑tactile exam of the lips, tongue, gums, cheeks, floor and roof of the mouth, and the neck. Dentists assess risk factors—tobacco, heavy alcohol use, HPV exposure, age over 40, and a family history—to decide how often a screening should occur (often annually, or every six months for high‑risk patients). Early‑stage disease is often asymptomatic; a persistent white or red patch, non‑healing ulcer, lump, or numbness that lasts more than two weeks should trigger a prompt biopsy. Detecting cancer while it is still localized boosts five‑year survival to 80‑90 %, compared with 30‑40 % for advanced disease. This dramatic survival benefit underscores why the American Dental Association recommends at least one oral‑cancer screen per year for all adults and more frequent exams for high‑risk individuals. In addition to professional exams, monthly self‑exams empower patients to notice changes between visits. Together, regular dental exams, risk‑factor counseling, and timely referral for biopsy form a proven strategy that saves lives and preserves oral function.
Routine dental visits are the frontline defense against oral cancer. Every comprehensive check‑up includes a visual‑tactile exam of the lips, tongue, gums, cheeks, floor and roof of the mouth, and the neck. Dentists assess risk factors—tobacco, heavy alcohol use, HPV exposure, age over 40, and a family history—to decide how often a screening should occur (often annually, or every six months for high‑risk patients). Early‑stage disease is often asymptomatic; a persistent white or red patch, non‑healing ulcer, lump, or numbness that lasts more than two weeks should trigger a prompt biopsy. Detecting cancer while it is still localized boosts five‑year survival to 80‑90 %, compared with 30‑40 % for advanced disease. This dramatic survival benefit underscores why the American Dental Association recommends at least one oral‑cancer screen per year for all adults and more frequent exams for high‑risk individuals. In addition to professional exams, monthly self‑exams empower patients to notice changes between visits. Together, regular dental exams, risk‑factor counseling, and timely referral for biopsy form a proven strategy that saves lives and preserves oral function.
Recognizing Early Warning Signs
Recognizing Early Warning Signs
| Sign | Typical Appearance / Symptom |
|---|---|
| Non‑healing ulcer | Persistent sore > 3 weeks, does not resolve. |
| Red or white patch | Leukoplakia (white) or erythroplakia (red/velvety). |
| Lump or thickening | Firm nodule on lip, tongue, inner cheek, or gums. |
| Pain/discomfort | Unexplained pain when chewing, swallowing, or speaking. |
| Swallowing difficulty | Sensation of food stuck, dysphagia. |
| Voice changes | Hoarse or croaky voice. |
| Neck swelling | Lump or swollen lymph node in neck/throat. |
 Detecting mouth cancer early saves lives, and patients can often spot the first clues themselves. What are the very first signs of mouth cancer? The earliest warning is usually a non‑healing ulcer that does not heal within three weeks. A flat white patch (leukoplakia) or a red, velvety area (erythroplakia on the cheek, tongue, or lip can also appear, as can a small, firm lump or thickening that feels different from the surrounding tissue. New or worsening pain when chewing or swallowing should raise concern.
Detecting mouth cancer early saves lives, and patients can often spot the first clues themselves. What are the very first signs of mouth cancer? The earliest warning is usually a non‑healing ulcer that does not heal within three weeks. A flat white patch (leukoplakia) or a red, velvety area (erythroplakia on the cheek, tongue, or lip can also appear, as can a small, firm lump or thickening that feels different from the surrounding tissue. New or worsening pain when chewing or swallowing should raise concern.
What are the 7 warning signs of mouth cancer? 1) Non‑healing ulcer or sore; 2) Persistent red or white patch; 3) Lump or thickening on lip, tongue, or inside the mouth; 4) Unexplained pain or discomfort; 5) Difficulty swallowing or a feeling of food stuck; 6) Hoarse or croaky voice; 7) Swelling or lump in the neck or throat.
First signs of mouth cancer pictures Visual examples include a shallow ulcer on the lower lip, a speckled lesion inside the cheek, a red‑velvety patch on the ventral tongue, and a well‑defined white lesion with irregular borders on the lateral tongue. Any of these that persist beyond two weeks merit a prompt dental evaluation.
Gum cancer symptoms Look for a persistent sore, lump, or ulcer on the gums that does not heal, white or red patches along the gumline, unexpected bleeding, firm swelling, numbness, or loose teeth.
Stage 1 oral cancer symptoms Usually limited to visual changes such as leukoplakia, erythroplakia, mixed red‑white patches, a non‑healing ulcer or a thickened spot on the inner cheek. Numbness is less common but may appear.
What is the biggest indicator of oral cancer? A lesion that does not heal within two weeks—especially a persistent ulcer or red/white patch—is the single most alarming sign and should trigger an immediate dental or medical assessment.
Self‑Exams and At‑Home Detection
Self‑Exams and At‑Home Detection
| Step | Action |
|---|---|
| Lighting | Stand under bright light, use a hand mirror. |
| Visual inspection | Examine lips, both sides of tongue (incl. underside), gums, roof/floor of mouth, inner cheeks for patches, sores, texture changes. |
| Tactile exam | Gently run clean fingertips over all areas and palpate neck/under jaw for lumps. |
| Timing | Perform monthly; any unchanged abnormality > 2 weeks → contact dentist. |
| Adjunctive tools | VELscope fluorescence or toluidine‑blue staining (optional, $19/visit). |
 Monthly self‑inspection is a simple, low‑cost habit that can dramatically improve early‑cancer detection. Each month, stand in front of a bright light and use a hand mirror to examine the lips, both sides of the tongue (including the underside), the gums, the roof and floor of the mouth, and the inner cheeks. Look for white or red patches, persistent sores, or any change in texture. Follow the visual check with a gentle tactile exam: run clean fingertips over each area and feel the neck and under the jaw for lumps or swollen lymph nodes. If anything remains unchanged for more than two weeks, call your dentist promptly for a professional evaluation.
Monthly self‑inspection is a simple, low‑cost habit that can dramatically improve early‑cancer detection. Each month, stand in front of a bright light and use a hand mirror to examine the lips, both sides of the tongue (including the underside), the gums, the roof and floor of the mouth, and the inner cheeks. Look for white or red patches, persistent sores, or any change in texture. Follow the visual check with a gentle tactile exam: run clean fingertips over each area and feel the neck and under the jaw for lumps or swollen lymph nodes. If anything remains unchanged for more than two weeks, call your dentist promptly for a professional evaluation.
The primary diagnostic tool used by clinicians is an oral cancer screening—a visual and tactile exam that may be enhanced with special lights (e.g., VELscope fluorescence) or dyes such as toluidine‑blue to highlight abnormal tissue. When a lesion looks suspicious, a biopsy (incisional, brush, or panendoscopic) is taken for histopathology; blood tests for oral cancer are still experimental and not part of routine care.
Cost considerations are minimal. Most comprehensive dental visits include the visual screen at no extra charge, and many insurers cover it. Adjunctive fluorescence screening with a VELscope device typically costs about $19 per visit, with some practices offering discounts or charitable contributions. Regular dental check‑ups combined with diligent self‑exams provide the most reliable, affordable strategy for early detection.
Professional Screening Tools and Adjuncts
Professional Screening Tools and Adjuncts
| Tool | Purpose / Use |
|---|---|
| Visual‑tactile exam | Standard screening during routine dental visit. |
| VELscope (blue‑light autofluorescence) | Highlights abnormal tissue (darker) vs healthy green glow. |
| Toluidine‑blue stain | Stains dysplastic cells for better visual contrast. |
| Dental hygienist questionnaire | Screens for tobacco use, voice changes, persistent sores. |
| Referral pathway | Dentist → oral/maxillofacial surgeon or ENT for biopsy → head‑and‑neck oncologist. |
 Routine dental visits are the front line for catching mouth cancer early. In our practice we use adjunctive visualization technologies such as blue‑light autofluorescence (e.g., VELscope®) that make abnormal tissue appear darker than the bright green glow of healthy mucosa, helping us spot lesions invisible under white light. Dental hygienists play a vital role: during cleanings they ask about tobacco use voice changes, and persistent sores, then perform a systematic visual‑tactile exam of the lips, tongue, floor of mouth, and neck. Any lesion that does not heal within two weeks is documented and flagged for further evaluation. When a suspicious area is identified, we follow a clear specialist referral pathway—first to an oral and maxillofacial surgeon or otolaryngologist for a definitive biopsy, then to a head‑and‑neck oncologist for staging and treatment planning. This coordinated approach ensures that early‑stage cancers (stage I‑II) are caught, where five‑year survival exceeds 80 %, giving patients the best chance for a cure and preserving oral function.
Routine dental visits are the front line for catching mouth cancer early. In our practice we use adjunctive visualization technologies such as blue‑light autofluorescence (e.g., VELscope®) that make abnormal tissue appear darker than the bright green glow of healthy mucosa, helping us spot lesions invisible under white light. Dental hygienists play a vital role: during cleanings they ask about tobacco use voice changes, and persistent sores, then perform a systematic visual‑tactile exam of the lips, tongue, floor of mouth, and neck. Any lesion that does not heal within two weeks is documented and flagged for further evaluation. When a suspicious area is identified, we follow a clear specialist referral pathway—first to an oral and maxillofacial surgeon or otolaryngologist for a definitive biopsy, then to a head‑and‑neck oncologist for staging and treatment planning. This coordinated approach ensures that early‑stage cancers (stage I‑II) are caught, where five‑year survival exceeds 80 %, giving patients the best chance for a cure and preserving oral function.
Understanding Cancer Staging and Prognosis
Understanding Cancer Staging and Prognosis
| Stage | Tumor Size / Extent | Node Involvement | Typical 5‑Year Survival |
|---|---|---|---|
| 0 (carcinoma in situ) | Confined to surface lining | None | > 95 % |
| I | ≤ 2 cm, no nodes | None | 80‑90 % |
| II | 2–4 cm or single nearby node | Single node (≤ 3 cm) | 70‑80 % |
| III | > 4 cm or multiple ipsilateral nodes | Multiple ipsilateral nodes | 50‑60 % |
| IVa | Large primary or extensive regional nodes, no distant mets | Regional nodes (any size) | 30‑45 % |
| IVb/c | Distant metastasis (lung, liver, etc.) | Distant nodes/metastases | < 30 % |
 Regular dental visits give dentists the chance to spot oral cancer early, and understanding the stage of the disease is key to planning treatment and predicting outcomes.
Regular dental visits give dentists the chance to spot oral cancer early, and understanding the stage of the disease is key to planning treatment and predicting outcomes.
Oral cancer stages – The American Joint Committee on Cancer (AJCC) uses the TNM system to classify oral cancers into five main stages. Stage 0 (carcinoma in situ) means abnormal cells are confined to the surface lining. Stage I describes a tumor ≤ 2 cm with no lymph‑node involvement or distant spread. Stage II involves a larger tumor (2–4 cm) or early spread to a single nearby lymph node. Stage III denotes an even larger tumor (> 4 cm) or multiple affected lymph nodes on the same side of the neck. Stage IV is the most advanced, including any size tumor that has spread to distant lymph nodes, adjacent structures, or distant organs such as the lungs or liver.
1st oral cancer stages – The earliest invasive stage is Stage I, where the tumor is small (≤ 2 cm) and confined to the oral mucosa. At this point the disease often appears as a persistent white or red patch, a non‑healing ulcer, or a thickened area that does not resolve within two weeks. Because the cancer is still localized, a simple biopsy and imaging are usually enough to confirm the diagnosis and guide treatment.
Oral cancer stages pictures – Visual references show the progression from subtle mucosal changes to extensive tissue invasion. Stage 0 lesions look like flat white (leukoplakia) or red (erythroplakia) patches without ulceration. Stage I appears as a small, well‑defined ulcer or lesion 2 cm. Stage II lesions are larger (2–4 cm) and may have indurated edges. Stage III shows irregular, ulcerated masses that may involve nearby structures such as the floor of the mouth or tongue. Stage IV cancers are extensive, often with jaw fixation, regional lymph‑node involvement, or distant metastasis.
Stage 4a oral cancer prognosis – This locally advanced stage (large primary tumor or extensive regional node involvement without distant spread) carries a 5‑year survival of roughly 30‑45 % in the United States. Outcomes improve with a multidisciplinary approach—surgery, radiation, and often chemotherapy—especially when patients are in good overall health.
Is stage 1 mouth cancer curable? – Yes. Stage I oral cancer is highly curable, with five‑year survival rates exceeding 80 % when treatment is started promptly. Surgical removal of the small, localized tumor—sometimes followed by a brief course of radiation or chemotherapy—offers an excellent chance of cure and return to normal oral function.
Early detection through routine dental exams, visual and tactile screening, and, when needed, adjunctive tools such as toluidine‑blue staining or fluorescence lighting dramatically improves the odds of catching the disease at Stage 0 or I, where treatment is most effective and less invasive.
Path to Diagnosis and Treatment
Path to Diagnosis and Treatment
| Phase | Procedure | Goal |
|---|---|---|
| Screening | Visual‑tactile exam (± adjunctive light/stain) | Identify suspicious lesions. |
| Biopsy | Brush, incisional, or fine‑needle biopsy | Obtain tissue for histopathology. |
| Imaging | CT, MRI, PET, ultrasound | Determine tumor depth, nodal spread, distant mets. |
| Staging | AJCC TNM classification | Guide treatment planning. |
| Treatment | Surgery ± radiation ± systemic therapy (chemo/targeted/immuno) | Remove disease, control local/regional spread. |
| Follow‑up | Regular exams, imaging, supportive care | Detect recurrence, preserve function. |
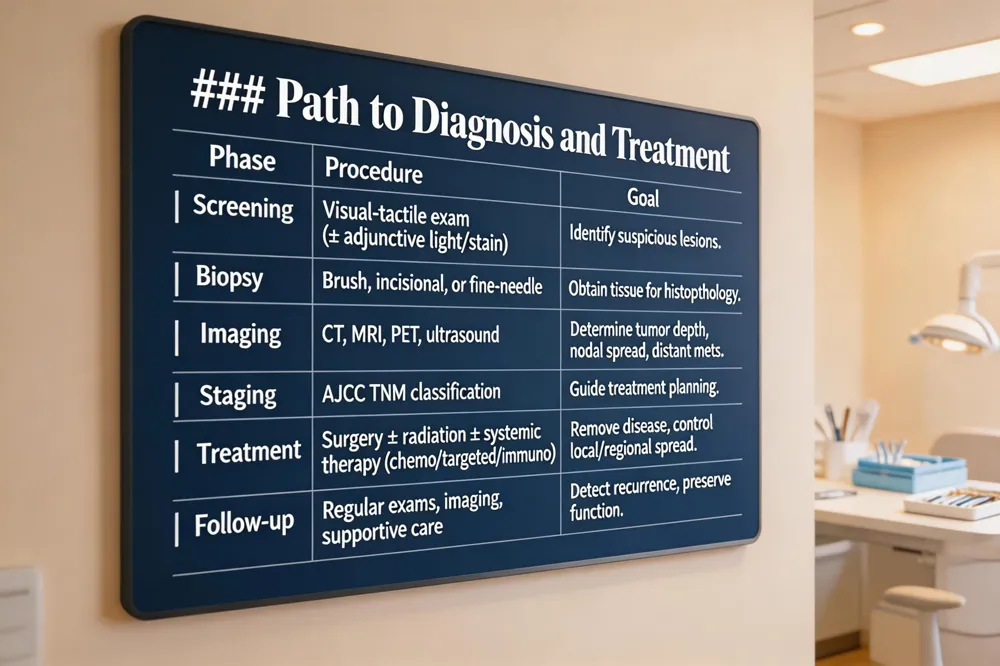 Diagnostic test for oral cancer
Diagnostic test for oral cancer
A diagnostic work‑up starts with a thorough visual and tactile exam of the lips, tongue, gums, cheek lining, floor and roof of the mouth during a routine dental visit. Suspicious white or red patches (e.g., leukoplakia, erythroplakia) prompt a brush biopsy or tissue biopsy. If cancer is confirmed, imaging—X‑ray, CT, MRI, or ultrasound—determines tumor depth and nodal spread, allowing rapid referral to an oral‑maxillofacial surgeon or oncologist.
Test for tongue cancer
Tongue evaluation follows the same visual‑palpation protocol, often supplemented by a thin‑tube endoscopy to view deeper tissue. Definitive diagnosis requires a biopsy (scalpel or fine‑needle). Staging imaging (CT, MRI, PET, ultrasound) maps tumor size and spread, guiding the specialist team.
Treatment for oral cancer
Management is multidisciplinary: surgery removes the primary lesion, radiation may follow or substitute when surgery isn’t feasible, and systemic therapies (chemotherapy, targeted agents, immunotherapy) address microscopic disease. Nutrition, speech, and emotional support are integrated into personalized care plans.
Can you die from mouth cancer
Yes. Five‑year survival exceeds 85 % for stage I disease but falls to ~35 % for stage IV. Early detection dramatically improves outcomes; late‑stage disease is far harder to cure.
What type of doctor do you see for oral cancer
First, a dentist or dental hygienist screens. Suspicious lesions lead to referral to an oral‑maxillofacial surgeon or head‑and‑neck (ENT) specialist for biopsy and staging, followed by an oncologist for radiation or systemic therapy.
Oral cancer screening near me
At Dr. Anthony P. Parrella’s Somerville office, every routine exam includes a comprehensive oral cancer screen with visual inspection, palpation, and optional adjunctive tools. Suspicious findings are brushed for cytology or promptly referred for biopsy. Call to schedule your screening today.
Can your dentist tell if you have oral cancer?
Yes. Dentists examine every oral surface for non‑healing sores, discolored patches, or lumps. Adjunctive lights or stains may highlight abnormal cells. If anything looks concerning, a biopsy is taken for definitive diagnosis, though the final confirmation comes from pathology.
Take Action Today
Schedule your next dental exam now—most dentists perform a quick, painless oral‑cancer screening during routine check‑ups. Perform a monthly self‑exam using a mirror, looking for persistent sores, white or red patches, lumps, or numbness, especially if you use tobacco or alcohol. Stay informed about risk factors such as tobacco, heavy drinking, HPV infection, and sun exposure, and discuss any concerns with your dentist to catch problems early.
